By Jim Myers, DPC Patient Ambassador.
By Jim Myers, DPC Patient Ambassador.
I had a conversation with my doctor last week. (My nephrologist, Dr. Vavilala, we call him Dr. V). He asked me if I had heard anything during my last trip to Washington, D.C. about an extension of coverage through the ACA to kidney transplant patients of the immunosuppressive drug coverage beyond the 36 month period that currently exists. This rang a bell in the back of my brain, so I decided to check it out.
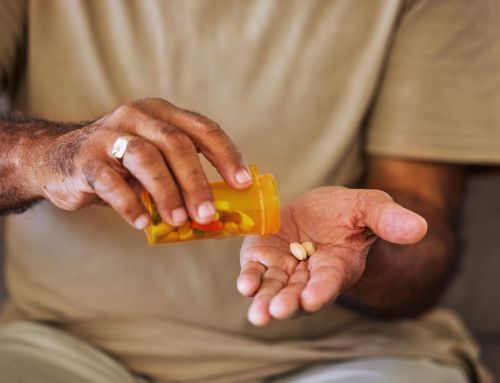
Every transplant patient or transplant candidate knows the current status of the law. If you are a kidney transplant recipient, you must take medications the rest of your life to prevent rejection of your transplanted kidney. Medicare pays for the transplant and immunosuppressive drugs for 36 months post-transplant, but coverage of these critical medications stops unless the beneficiary is Medicare-aged or Medicare-disabled. Here is where the gap in coverage comes in; if you’re under 65 and you have received a transplant, you are not age-eligible, nor are you considered disabled because after you have a transplant, you are no longer Medicare-disabled. Coverage for anti-rejection drugs for those patients that fall into the gap is limited to 36 months. The catch is that anti-rejection meds are very expensive. One newspaper article I read reports that one patient was paying as much as $1,750 a month, and the National Kidney Foundation estimates that Medicare pays $124,643 for a first year transplant patient, and then pays $24,612 a year primarily for anti-rejection meds thereafter.
So what happens to the transplant patient who has to make the choice between heating, eating & driving or taking his immunosuppressive medications? An all too common scenario for those that fall into the gap is they skip their meds, their newly implanted kidneys fail, and they end up back on dialysis.
This is particularly maddening when you consider that your life expectancy on dialysis is about 5 years and your life expectancy from a live transplant can be 12-20 years, with a much better quality of life. This is particularly striking when you consider that some transplants have lasted as long as 40 years.
Another big factor to consider is costs. The National Kidney Foundation makes the following comparison between the cost of a transplant and the costs of dialysis:
Medicare spends an average of $86,316 per year for an individual who is on dialysis and $124,643 during the first year of a kidney transplant. However, after the year of transplant, the cost is much lower at $24,612 for an individual with a functioning kidney transplant. If the transplant fails, the patient returns to dialysis or receives another transplant, each covered again by Medicare.
Think about that for a minute; almost a $60,000/year savings by simply preserving and protecting a transplanted kidney! The NKF has proposed legislation for years to plug this gap, but despite wide-spread acceptance, the bill has yet to become law.
To answer the doctor’s question, we look to the NKF blog on the subject:
We are confident that the declining cost of the drugs, coupled with the fact that many currently uninsured transplant recipients will be able to purchase insurance under the Affordable Care Act (ACA), will make H.R. 1428 / S. 323 very cost effective and increases the possibility of congressional approval. The CRS study reviewed preliminary information on the ACA’s essential health benefits (EHB) benchmark plan in multiple states, and found that the plans will typically require health plans to cover these immuno drugs. Thus, since more people will have insurance coverage, fewer will need the extended Medicare benefit, lowering the cost of H.R. 1428 / S. 323.”
In other words, in the opinion of the National Kidney Foundation, the ACA may now cover that gap in coverage for the immunosuppressant drugs, extending the 36 months in coverage to coverage for a lifetime. The NKF has made clear that they are still pursuing a bill to extend this coverage and preventing insurance carriers from cancelling you once you have coverage.
I then located the study referred to in the NKF blog. The article notes that in 2007, the Government Accountability Office (GOA) found the percentage of kidney transplant failures had nearly doubled when examining the results after a 7 year period, post-transplant. The study attributed at least part of this failure to patients not taking anti-rejection meds due to prohibitive costs after the 36 month period had run. The article notes that beginning in 2014, patients with a kidney transplant who are no longer entitled to Medicare payments for their anti-rejection meds may have access to extended coverage under the ACA. The CRS paper went on to note that a random sampling of plans covered prescription drugs, presumably including immunosuppression drugs used by ESRD patients to prevent transplanted kidney rejection. More to the point, the ACA beginning in 2014 requires private health plans offered through exchanges to cover essential health benefits (EHB). The 2012 benchmark standards require all plans available in exchanges to cover drugs in the immunosuppressive class. What this means in plain English is that somewhere between 3-24 anti-rejection drugs and roughly 20 products must be covered by state exchanges including common immunosuppressive drugs used by kidney transplant recipients. This comes as potentially good news for kidney transplant patients!
Click here to send a letter to your legislators to support immunosuppressive drug coverage today!